Samenvatting
Achtergrond
Alcoholhallucinose is een zeldzame complicatie van de diagnose ‘stoornis in alcoholgebruik’, gekenmerkt door acuut ontstane hallucinaties tijdens of na een periode van alcoholgebruik. De hallucinaties kunnen lang aanhouden, waardoor het beeld kan worden verward met een schizofreniespectrumstoornis. De prognose is meestal gunstig, maar als patiënten niet behandeld worden, is het mortaliteitsrisico aanzienlijk (37% in 8 jaar).
Casus
Een 38-jarige man werd opgenomen in een psychiatrisch ziekenhuis wegens hallucinaties die ontstonden tijdens alcoholgebruik en die 2 maanden na abstinentie aanhielden. Patiënt ervoer visuele, auditieve en tactiele hallucinaties, waarbij het bewustzijn, de aandacht, de oriëntatie en de hogere cognitieve functies intact bleven. Lichamelijk en beeldvormend onderzoek lieten geen afwijkingen zien. Patiënt herstelde gedeeltelijk na behandeling met haloperidol.
Conclusie
Bij hallucinaties tijdens of na een periode van alcoholgebruik moet de diagnose ‘alcoholhallucinose’ worden overwogen. Deze diagnose dient te worden onderscheiden van een delirium tremens en een schizofreniespectrumstoornis, omdat de behandeling en prognose ervan op wezenlijke punten verschillen.
Leerdoelen
- Alcoholhallucinose wordt gekenmerkt door een acuut ontstaan van vaak auditieve hallucinaties tijdens of na een periode van alcoholgebruik.
- De pathofysiologie van alcoholhallucinose is grotendeels onbekend, maar beeldvormend onderzoek laat hypometabolisme van de thalamus en hypofrontaliteit zien.
- Alcoholhallucinose dient niet te worden verward met schizofrenie of een delirium tremens.
- De 8-jaarsmortaliteit van alcoholhallucinose is 37%, met name door suïcide.
- Antipsychotica zijn de behandeling van eerste keus bij patiënten met alcoholhallucinose; daarnaast worden ook goede resultaten bereikt met valproïnezuur.
- Bij volledige remissie van alcoholhallucinose en abstinentie is continuering van de antipsychotische medicatie onnodig.
artikel
Inleiding
Alcoholhallucinose is een psychotische stoornis door alcoholgebruik en is een zeldzame complicatie van de diagnose ‘stoornis in alcoholgebruik’. Deze neuropsychiatrische aandoening kenmerkt zich door een acuut ontstaan van hallucinaties, vaak auditief van aard, na of tijdens een periode van alcoholgebruik.1,2 Hoewel beschrijvingen van het klinisch beeld teruggaan tot de 19e eeuw, is de pathofysiologie ervan nog onopgehelderd.3 De 10-jaarsprevalentie van alcoholhallucinose bij patiënten met een stoornis in alcoholgebruik ligt rond 0,4-0,7%, met een gemiddeld begin op de leeftijd van 35-50 jaar.1,4-6
In dit artikel beschrijven wij een man die tijdens alcoholdetoxificatie hallucinaties ervoer die aanhielden gedurende 2 maanden van abstinentie.
Ziektegeschiedenis
Patiënt A, een 38-jarige man, werd vrijwillig opgenomen op een verslavingsafdeling voor alcoholdetoxificatie en het afwenden van suïcidaliteit. Zijn voorgeschiedenis vermeldde een alcoholonttrekkingsinsult, meerdere depressieve episoden met tentamina suicidii en 2 bypassoperaties wegens myocardinfarcten. Patiënt gebruikte sinds zijn 20e levensjaar alcohol, van dagelijks een halve fles whisky tot een liter gedurende de laatste 5 jaar. Andere verdovende middelen gebruikte hij niet. Wel gebruikte hij de volgende medicatie: pantoprazol, amlodipine, atorvastatine, clopidogrel, valsartan, metoprolol, acetylsalicylzuur, venlafaxine, natriumvalproaat, hydrochloorthiazide, zopiclon en promethazine. Jaren geleden verloor hij zijn werk, zijn relatie en zijn woning. De laatste 10 jaar werd hij bijna halfjaarlijks opgenomen in verslavingsklinieken, waar hij meestal vroegtijdig met ontslag ging en ondanks zijn lichamelijke klachten terugviel in alcoholgebruik. Ook patiënts vader en enkele andere familieleden hadden een stoornis in alcoholgebruik.
Tijdens de detoxificatieperiode begonnen we met behandeling van patiënt met chloordiazepoxide 25 mg volgens het CIWA-Ar-protocol (CIWA-Ar staat voor ‘Clinical institute withdrawal assessment for alcohol, revised’). De eerste 3 dagen kreeg hij dagelijks thiamine 250 mg intramusculair en daarna 25 mg 3 dd oraal, plus vitamine C en vitamine B complex forte 500 mg 1 dd. In het eerste etmaal ervoer hij forse onttrekkingsverschijnselen, met CIWA-scores van 25-30; deze score daalde binnen 24 h tot < 10 (de CIWA-scoreschaal loopt van 0-67, waarbij een score < 10 betekent ‘geen of minimale onthoudingsverschijnselen’ en een score > 20 betekent ‘ernstige onthoudingsverschijnselen’).
Na ruim 1 week kreeg patiënt hallucinaties, die toenamen naarmate de abstinentie voortduurde. Zo zag patiënt zwermen vliegen, vlinders, bijen, kakkerlakken en andere beestjes in de ruimte (visuele hallucinaties, zoöpsie), voelde hij deze op de huid (tactiele hallucinaties) en onder de huid (formicatieve hallucinaties), en hoorde hij stemmen die in verschillende talen tegen hem spraken en simpele opdrachten gaven.
Bij psychiatrisch onderzoek zagen we een coöperatieve en verzorgde man met een helder bewustzijn, zonder aandachts- of denkstoornissen; de hogere cognitieve functies waren intact. Bij neurologisch onderzoek zagen we geen oogbewegingsstoornissen, ataxie of verwardheid, waarmee een Wernicke-encefalopathie minder waarschijnlijk werd. Er waren geen andere neurologische afwijkingen. 1,5 maand vóór de opname was een CT-scan gemaakt na een trauma capitis, waarop geen afwijkingen te zien waren. Ook een persisterend delier bij cerebrale schade was daarom onwaarschijnlijk. Laboratoriumonderzoek liet geen afwijkingen zien, behalve een verhoogde waarde van γ-GT. Om een – zeldzame – epileptogene genese van de hallucinaties uit te sluiten werd een eeg verricht, maar dit was evenmin afwijkend. Daar patiënt inmiddels enkele maanden abstinent was, bewustzijns- en aandachtsstoornissen ontbraken en de laboratoriumuitslagen vrijwel ongestoord waren, werd een delier al dan niet veroorzaakt door alcoholonttrekking uitgesloten. Het ontbreken van waanideeën en negatieve symptomen en het ontstaan van hallucinaties op latere leeftijd maakten schizofrenie onwaarschijnlijk. Omdat anhedonie en stemmingsstoornissen ontbraken, verwierpen we ook de diagnose ‘psychotische depressie’ en stelden de diagnose ‘psychotische stoornis op basis van alcoholgebruik’ (alcoholhallucinose).
Patiënt werd achtereenvolgens behandeld met quetiapine 600 mg en flupentixol 2 mg, beide 1 dd oraal, maar hierop persisteerden de hallucinaties. De flupentixol werd daarom vervangen door haloperidol 3 mg 1 dd oraal, waarop de intensiteit van de hallucinaties in 2 weken afnam. Vanuit de kliniek vertrok patiënt naar het buitenland, waar hij langere tijd zou verblijven.
Beschouwing
Diagnostiek en differentiaaldiagnose
De diagnose ‘alcoholhallucinose’ wordt gesteld op grond van opvallende hallucinaties die ontstaan tijdens een alcoholintoxicatie of binnen 1 maand erna. Differentiaaldiagnostisch staat het alcoholonttrekkingsdelier (delirium tremens) op de eerste plaats. Bij alcoholhallucinose is evenwel sprake van een helder bewustzijn, intacte oriëntatie en aandacht, afwezige of minimale ontwenningsverschijnselen en zijn er meestal meer auditieve dan visuele hallucinaties.2,4,7 Ook is het beloop vaak langduriger (tabel).2
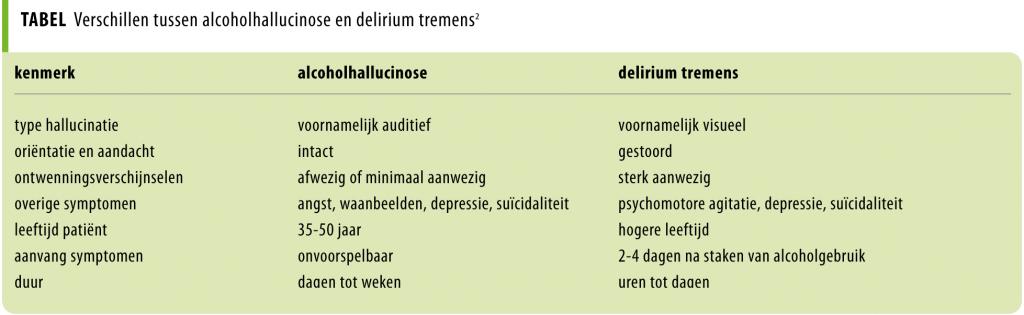
Alcoholhallucinose onderscheidt zich van schizofreniespectrumstoornissen door de afwezigheid van negatieve symptomen en desorganisatie, en omdat de aandoening zich veelal op latere leeftijd manifesteert.1,2 In de praktijk is het onderscheid echter niet altijd eenvoudig te maken.
Pathofysiologie
De pathofysiologie van alcoholhallucinose is maar gedeeltelijk bekend. Net als bij het delirium tremens lijkt het gamma-aminoboterzuur(GABA)-erge systeem een rol te spelen. Kleinschalige beeldvormende studies met PET en ‘single photon emission’-CT (SPECT) suggereren bovendien hypometabolisme van de thalamus en hypofrontaliteit. Volgens sommige auteurs is deze hypofrontaliteit te vergelijken met die bij schizofreniespectrumstoornissen en zou er sprake zijn van een pathofysiologisch continuüm.7,8
Behandeling
Hoewel er geen geprotocolleerde behandeling bestaat voor patiënten met alcoholhallucinose, vormen antipsychotica de behandeling van eerste keus. Patiëntenbeschrijvingen en -series laten een positief effect zien van behandeling met haloperidol, flupentixol, risperidon en valproïnezuur.3,4,9,10 Het alcoholgebruik dient uiteraard te worden gestaakt en vitamine B1 dient te worden gesuppleerd om microvasculaire schade in het brein en ontwikkeling van het syndroom van Wernicke te voorkomen. Benzodiazepinen kunnen worden overwogen bij patiënten met angst en onrust. Ten slotte wordt terugvalpreventie aanbevolen.
Prognose
Bij adequate behandeling vindt meestal een complete remissie van de hallucinaties plaats binnen enkele dagen tot weken. Bij abstinentie en volledige remissie bestaat geen noodzaak tot verdere antipsychotische behandeling. Van chronische alcoholhallucinose, waarbij de hallucinaties langer dan 6 maanden aanhouden, is geen prognose bekend. Wel kent alcoholhallucinose een hoge mortaliteit (37% in 8 jaar), met een hazardratio die 12 maal hoger is dan bij een geïsoleerde stoornis in alcoholgebruik.
Bekende doodsoorzaken van alcoholhallucinose zijn cardiovasculaire en andere somatische ziekten, maar vooral suïcide. Het risico op suïcide is zeker bij patiënten met een comorbide angststoornis of depressieve stoornis sterk verhoogd.2
Conclusie
Als een patiënt hallucinaties heeft tijdens of na een periode van alcoholgebruik, moet de diagnose ‘alcoholhallucinose’ worden overwogen. Deze diagnose onderscheidt zich van schizofrenie en delirium tremens op basis van de symptomen. Dit onderscheid is niet altijd eenvoudig te maken, maar heeft wel degelijk consequenties voor de duur van de behandeling en de prognose.
Literatuur
Jordaan GP, Nel DG, Hewlett RH, Emsley R. Alcohol-induced psychotic disorder: a comparative study on the clinical characteristics of patients with alcohol dependence and schizophrenia. J Stud Alcohol Drugs. 2009;70:870-6 Medline.
Jordaan GP, Emsley R. Alcohol-induced psychotic disorder: A review. Metab Brain Dis. 2014;29:231-43. Medline.
Bhat PS, Ryali V, Srivastava K, Kumar SR, Prakash J, Singal A. Alcoholic hallucinosis. Ind Psychiatry J. 2012;21:155-7. doi:10.4103/0972-6748.119646Medline
Soyka M, Täschner B, Clausius N. Neuroleptic treatment of alcohol hallucinosis: case series. Pharmacopsychiatry. 2007;40:291-2. doi:10.1055/s-2007-992144Medline
Perme B, Vijaysagar KJ, Chandrasekharan R. Follow-up study of alcoholic hallucinosis. Indian J Psychiatry. 2003;45:244-6 Medline.
Soyka M. Pharmacological treatment of alcohol hallucinosis. Alcohol Alcohol. 2008;43:719-20. doi:10.1093/alcalc/agn068Medline
Soyka M, Koch W, Tatsch K. Thalamic hypofunction in alcohol hallucinosis: FDG PET findings. Psychiatry Res. 2005;139:259-62. doi:10.1016/j.pscychresns.2005.05.009Medline
Kitabayashi Y, Narumoto J, Shibata K, Ueda H, Fukui K. Neuropsychiatric background of alcohol hallucinosis: a SPECT study. J Neuropsychiatry Clin Neurosci. 2007;19:85. doi:10.1176/jnp.2007.19.1.85Medline
De Millas W, Haasen C. Treatment of alcohol hallucinosis with risperidone. Am J Addict. 2007;16:249-50. doi:10.1080/10550490701375269Medline
Aliyev ZN, Aliyev NA. Valproate treatment of acute alcohol hallucinosis: a double-blind, placebo-controlled study. Alcohol Alcohol. 2008;43:456-9. doi:10.1093/alcalc/agn043Medline





Reacties